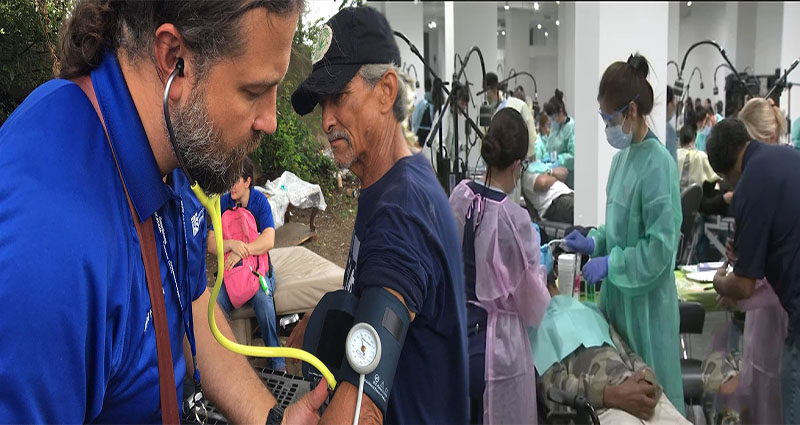
If you or someone you know is homeless, you may not realize that there is a health care center specifically for the homeless. These facilities provide basic primary care, including preventative care for medical issues like high blood pressure, developmental delays, emotional disability, and long-term care. Depending on the needs of your community, you may be able to find the right care at a health care center for the homeless. Here are some of these programs in action.
Community First Health Centers Homeless Health Care Program
The Community First Health Centers Homeless Wellness Program is a comprehensive approach to the health care needs of the homeless. The program offers behavioral and medical assessments, transportation, and mental health services. Its services include primary care, dental, and vision care, as well as access to WIC and language translation services.
Approximately half of the homeless people served by Community First’s program are women. Community First is committed to providing high-quality care to all homeless individuals.
The program provides comprehensive health care for the homeless population in St. Clair and Macomb Counties. Staff recognize the challenges of living among the homeless and its impact on their health. The program uses a team approach to care for the homeless, with a variety of disciplines and supervised volunteers. Community First’s team of providers is highly qualified to diagnose and treat a variety of illnesses, including mental health issues and substance abuse disorders.
HOPE team
The HOPE team at a health care center for homeless provides assistance to the most vulnerable population of the community. They help clients access mainstream benefits such as food stamps, medical care, and other services. They also offer transportation and outreach to meet client needs. HOPE teams are active participants in the Housing First model. Their mission is to create a better community for those in need. The health care center for homeless works with local nonprofits and other community organizations to improve the lives of the homeless.
One such initiative is medical respite, which costs much less than hospital care. It helps extend the lives of homeless residents by discovering chronic conditions that might otherwise remain undetected. One Washington, DC, health care provider, AmeriHealth Caritas DC, recently sent 11 homeless patients to its Hope Has a Home clinic. The number of primary care visits skyrocketed, sending total costs up 75 percent. In the coming years, AmeriHealth plans to open two medical respite centers for the homeless.
Shelter-based clinics
The Health Care of Homeless Persons Manual identifies common serious health problems experienced by homeless people and describes appropriate treatments. It also describes current practices and best practices for collaborating effectively with shelter staff and providing trauma-
informed care. This guide is written for communities of health care service providers who are trying to meet the needs of homeless people. Although it is not a step-by-step guide for establishing shelter-based clinics, it will be a valuable resource for practitioners and organizations interested in providing health care to the homeless.
There were several models for providing health care to the homeless before the mid-1980s. Several of these programs were deemed successful and the main impetus for the implementation of Title VI of the Stewart B. McKinney Homeless Assistance Act in 1987. These projects helped establish a benchmark for future homeless health care programs. The research team developed a shelter-based health clinic model and collected clinical measures for youth during its operation between October 2016 and June 2018.
Intensive residential programs
A new study from the National Institute for Medical Respite Care highlights the importance of IMCCs in homeless health. The report, “State of Medical Respite/Recuperative Care Programs: A Comprehensive Approach to Health Care for the Homeless,” details the benefits of such programs. The study’s authors, Suzanne Zerger and Bruce Doblin, highlight three programs that provide a holistic approach to health care for the homeless.
Two shelter-based collaborative mental health care models, IMCC and SOCC, were studied. Results of the study sample revealed that participants in both models experienced improvements in housing, health care utilization, and community functioning. The study also found that the less resource-intensive SOCC care model was not associated with any significant differences in outcomes. These results suggest that both models of care improve mental health outcomes for homeless men.